An evidence-based overview presents practical, low-cost meal ideas that reduce dietary drivers of chronic inflammation. It summarizes simple plate rules, pantry staples, and breakfast-to-dinner templates grounded in human and clinical nutrition findings. The tone remains measured and supportive, emphasizing actionable swaps and modest habits that accumulate benefits. Practical tips on shopping, flavoring, and tracking symptoms follow, offering clear next steps for anyone ready to begin.
What an Anti-Inflammatory Diet Means

Rooted in clinical research and nutritional science, an anti-inflammatory diet emphasizes foods that lower chronic inflammation markers—such as omega-3–rich fish, a variety of vegetables and fruits, whole grains, nuts, and legumes—while limiting pro-inflammatory items like processed foods, refined sugars, and excess red or processed meats.
It prioritizes nutrient density, fiber, antioxidants, and unsaturated fats to modulate immune signaling and oxidative stress.
Evidence links such patterns to lower C-reactive protein and improved metabolic profiles.
Implementation is individualized, considering comorbidities, medications, and preferences.
The approach complements medical care, supporting measurable biomarkers and functional outcomes rather than promising cure-all effects.
Make sure to stock pantry staples like olive oil, canned beans, and whole grains to support consistent meal preparation and adherence to the diet, including essential foods that appear on recommended grocery lists.
Quick Rules: Build an Anti-Inflammatory Plate

Consistently, an anti-inflammatory plate centers on three simple proportions: half filled with a variety of colorful vegetables and fruit, a quarter with lean protein (preferably fatty fish, poultry, legumes, or nuts), and a quarter with whole grains or starchy vegetables, while replacing added sugars, highly processed foods, and trans fats with sources of unsaturated fat such as olive oil and avocado. Evidence favors fiber, omega-3s, polyphenols, and low glycemic load. Practical tips include portion cues, varied colors, and cooking methods that preserve nutrients. For shopping and meal prep, stock up on whole grains, fatty fish, legumes, nuts, olive oil, and a rainbow of produce to follow an anti-inflammation diet.
| Component | Examples | Benefits |
|---|---|---|
| Vegetables/Fruit | Berries, leafy greens, peppers | Fiber, antioxidants |
| Protein | Salmon, lentils, chicken | Omega-3s, amino acids |
| Grains/Fats | Quinoa, sweet potato, olive oil | Whole grains, unsaturated fats |
Pantry Staples to Stock for Inflammation-Fighting Meals

A well-stocked pantry supports consistent anti-inflammatory eating by prioritizing whole grains and legumes, which provide fiber, resistant starches, and plant protein linked to reduced markers of inflammation.
Staples such as quinoa, oats, brown rice, lentils, and chickpeas offer versatile bases for meals and sustained blood-sugar control. Complementing these are anti-inflammatory spices—turmeric, ginger, cinnamon, and black pepper—that have bioactive compounds shown in clinical and preclinical studies to modulate inflammatory pathways. Adding fatty fish and nuts can further reduce inflammation by providing omega-3 fatty acids health benefits that have been associated with lower inflammatory markers.
Whole Grains & Legumes
Among pantry staples, whole grains and legumes stand out for their documented anti-inflammatory benefits: high fiber, resistant starch, and plant protein support gut microbiota diversity and lower circulating inflammatory markers in multiple clinical and observational studies.
Practical options include oats, barley, brown rice, quinoa, lentils, chickpeas, and various beans, chosen for nutrient density and low processing.
Regular intake correlates with improved glycemic control, favorable lipid profiles, and reduced systemic inflammation in randomized and cohort research.
Preparation tips—soaking, proper cooking, pairing with polyphenol-rich vegetables—enhance digestibility and bioavailability, making these staples reliable, evidence-backed components of an anti-inflammatory pantry.
Including a variety of whole grains and legumes also helps increase fiber intake and overall nutrient diversity.
Anti-Inflammatory Spices
Building on pantry foundations like whole grains and legumes, a small selection of spices can markedly amplify a meal’s anti-inflammatory potential by delivering concentrated bioactive compounds such as curcumin, eugenol, and gingerols.
Turmeric (curcumin) pairs with black pepper for absorption; ginger provides gingerols and shogaols that modulate cytokine activity; cloves and cinnamon supply eugenol and cinnamaldehyde with antioxidant effects.
Oregano, rosemary, and thyme contribute polyphenols; chili peppers offer capsaicin for neurogenic inflammation modulation.
Store whole spices for longevity, grind fresh when possible, and integrate them routinely to support dietary inflammation reduction alongside overall healthy patterns.
Including anti-inflammatory soups like turmeric-ginger broth can be an easy way to combine these ingredients for soothing, nutrient-dense meals with anti-inflammatory benefits.
Foods and Drinks to Limit or Avoid

Frequently, clinicians and nutrition researchers recommend limiting certain foods and beverages that promote inflammation because consistent evidence links them to increased inflammatory markers, metabolic dysregulation, and heightened chronic disease risk.
Practical guidance emphasizes reducing items high in added sugars, refined grains, and industrial trans fats while moderating alcohol and processed red meats. Choosing whole foods, fiber, and unsaturated fats supports inflammatory balance. Incremental substitutions (e.g., fruit for sugary snacks) yield measurable biomarker improvements.
Clear labeling, portion control, and mindful eating help adherence. Suggested items to limit or avoid include:
- Sugary beverages and fruit drinks
- Refined white breads and pastries
- Processed meats (sausages, deli meats)
- Trans-fat-containing packaged snacks
- Excessive alcohol
Clinicians often recommend following an anti-inflammatory diet as a practical approach to reduce chronic inflammation and related health risks.
Breakfast Templates to Rotate All Week

Morning choices that pair balanced protein sources with healthy fats and fiber support blood sugar regulation and reduced inflammatory signaling.
Including anti-inflammatory grains such as oats, quinoa, and buckwheat provides whole‑grain carbohydrates and phytonutrients linked to lower markers of inflammation.
Easy smoothie bowls that combine leafy greens, berries, protein, and a sprinkle of seeds offer a convenient, nutrient‑dense template to rotate through the week.
Many of these options are simple to prepare and can become part of morning routines that help sustain energy and reduce inflammation.
Balanced Protein Starts
When protein is paired with fiber and anti-inflammatory fats at breakfast, physiological satiety signals stabilize blood glucose and reduce postprandial inflammation, supporting cognitive focus and metabolic resilience through the morning hours.
The section outlines morning templates emphasizing lean protein, plant-based options, and omega-rich fats to lower inflammatory markers and preserve muscle. Portions are pragmatic, evidence-aligned, and simple to rotate for variety.
Each template balances amino acids, soluble fiber, and monounsaturated or omega-3 sources to modulate insulin response and inflammatory cytokines while promoting sustained energy.
- Greek yogurt with berries and walnut sprinkle
- Soft-scrambled eggs with avocado
- Smoked salmon on cucumber rounds
- Chickpea scramble with spinach
- Cottage cheese with flax and apple
Anti-Inflammatory Grains
Built around whole grains with proven anti-inflammatory properties, these breakfast templates prioritize soluble fiber, low glycemic load, and phytonutrient-rich additions to blunt postprandial cytokine spikes and support gut barrier integrity.
Oats, barley, and quinoa provide beta-glucans and resistant starch that feed beneficial microbiota, reduce endotoxemia, and moderate glycemic response. Combine with nuts or seeds for omega-3s and polyphenols, and top with berries or citrus for anthocyanins and vitamin C to enhance antioxidant defenses.
Portion control and minimal added sugars preserve metabolic benefits. Rotating these grain bowls across the week sustains dietary diversity linked to lower systemic inflammation.
Easy Smoothie Bowls
As a quick, nutrient-dense option, smoothie bowls combine anti-inflammatory ingredients in a form that supports satiety, glycemic control, and gut health.
They layer fiber, omega-3s, polyphenols, and probiotic-supporting components to reduce postprandial inflammation and stabilize energy.
Templates emphasize low-glycemic fruits, leafy greens, unsweetened plant milk, and a protein or seed source to blunt glucose spikes.
Toppings add texture and targeted nutrients without excess sugar.
- Base: frozen berries, spinach, unsweetened almond milk
- Protein: Greek yogurt or pea protein
- Fats: ground flaxseed or chia
- Flavor: turmeric, cinnamon, ginger
- Texture: chopped nuts, sliced kiwi
Lunch Ideas for Workdays and Leftovers

Typically, practical workday lunches prioritize balance and anti-inflammatory ingredients—lean proteins, fiber-rich whole grains, healthy fats, and colorful vegetables—because research links these components to reduced systemic inflammation and improved metabolic markers.
Meal-prep options include grilled salmon or chickpea salads with quinoa, mixed greens, avocado, and turmeric vinaigrette for omega-3s, fiber, and polyphenols. Leftovers from batch-cooked stews or roasted vegetables pair well with brown rice or farro for sustained glycemic control.
Emphasis on portioned containers, minimal added sugars, and varied spices supports adherence. Clear labeling and rotating recipes reduce monotony while maintaining consistent anti-inflammatory nutrient intake.
Dinners You Can Make in 30 Minutes

Workday lunches that rely on batch-cooked proteins and whole grains naturally lead into evening meals that are both anti-inflammatory and time-efficient; dinners prepared in 30 minutes focus on nutrient-dense ingredients—lean fish, legumes, cruciferous vegetables, whole grains, and anti-inflammatory spices like turmeric and ginger—that research associates with lower markers of inflammation.
Evidence-based recipes emphasize quick methods: pan-searing, steaming, stir-frying, or sheet-pan roasting to preserve micronutrients and bioactive compounds. Meals minimize refined sugars and processed oils, favoring olive oil and omega-3 sources. Practical guidance supports consistent intake of polyphenols and fiber for measurable inflammatory benefit.
- Salmon with quinoa and steamed broccoli
- Lentil and spinach curry with brown rice
- Turmeric-ginger shrimp stir-fry with snap peas
- Chickpea and roasted cauliflower salad with tahini
- Sautéed kale, wild rice, and grilled mackerel
Kid- and Family-Friendly Swaps for Lower Inflammation

For families aiming to reduce dietary inflammation, practical swaps can make a measurable difference without sacrificing taste or convenience.
Replacing processed snacks with whole-food options, emphasizing a variety of colorful vegetables, and selecting whole-grain alternatives are supported by evidence to lower pro-inflammatory markers and improve nutrient density.
These changes can be implemented gradually with kid-friendly recipes and simple pantry substitutions to increase adherence and long-term benefit.
Swap Processed Snacks
Often overlooked, snack choices can meaningfully influence inflammatory markers, so replacing highly processed, sugar- and refined-grain–heavy options with minimally processed alternatives supports a lower-inflammatory dietary pattern for children and families.
Evidence-based swaps reduce added sugars, refined carbs, and industrial trans fats while increasing fiber, protein, and healthy fats that modulate inflammatory pathways.
Practical choices are portable, familiar, and acceptable to kids, easing family adoption. Portion guidance and routine (snack timing, pairing protein with carbohydrate) further stabilize blood sugar and inflammation-related responses. Small, consistent changes yield measurable benefits over time.
- Apple slices with nut butter
- Plain yogurt with berries
- Roasted chickpeas
- Whole-grain crackers with hummus
- Fresh fruit and cheese
Choose Colorful Veggies
After swapping processed snacks for whole-food options, the next practical step emphasizes colorful vegetables as regular, kid-friendly components of meals and snacks to lower inflammation. Caregivers are advised to introduce a variety of phytonutrient-rich choices—red peppers, spinach, carrots, broccoli, and berries alongside vegetables—to provide antioxidants and fiber linked to reduced inflammatory markers. Simple preparations (roasted sticks, steamed florets, blended soups) increase acceptance while preserving nutrients. Portioning, dipping with yogurt-based sauces, and modeling consumption reinforce habits. Evidence supports diverse plant colors for complementary anti-inflammatory compounds; gradual inclusion and predictable presentation improve family uptake and sustained benefit.
Use Whole-Grain Alternatives
When swapped into everyday meals, whole-grain alternatives can lower dietary inflammation by increasing fiber, micronutrients, and bioactive compounds that modulate gut microbiota and systemic inflammatory markers.
Evidence-based guidance encourages replacing refined grains with whole options to support satiety, glycemic control, and anti-inflammatory pathways.
For families, gradual swaps and familiar textures improve acceptance while preserving nutrient density.
- Swap white rice for brown rice or barley
- Choose whole-wheat or spelt pasta over refined varieties
- Offer whole-grain breads and tortillas for sandwiches and wraps
- Use oats or quinoa in breakfasts and baking
- Mix whole-grain flours into pancakes and muffins
Smart Snacks and Smoothies for Steady Energy

Regularly incorporating nutrient-dense snacks and well-balanced smoothies can help maintain stable blood glucose, reduce inflammatory signaling, and prevent the energy crashes that drive poor food choices. Evidence supports combining fiber, lean protein, and healthy fats—for example, Greek yogurt with berries and walnuts or hummus with carrot sticks—to blunt postprandial glucose spikes and lower cytokine responses.
Smoothies blending leafy greens, a small portion of fruit, plant-based protein, and omega-3–rich seeds provide portable, anti-inflammatory nutrition without rapid glycemic load. Portion control and minimal added sugars maximize benefits. Strategic snacking preserves metabolic resilience, supports cognitive focus, and complements overall anti-inflammatory dietary patterns.
One-Week Anti-Inflammatory Meal Plan to Start Now
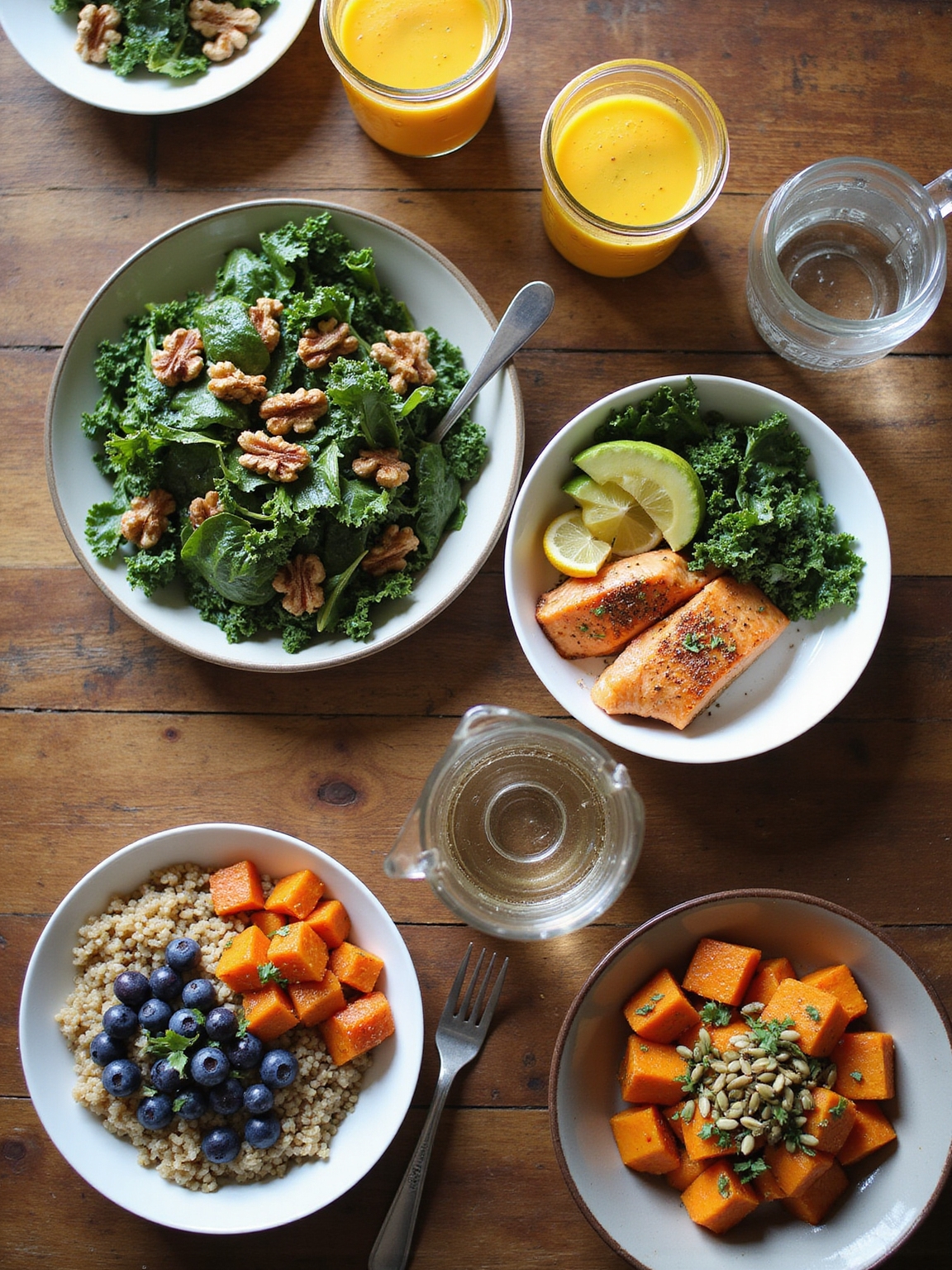
A one-week anti-inflammatory meal plan can orient morning choices toward nutrient-dense breakfasts—such as oatmeal with berries and walnuts or turmeric-spiced smoothies—that support glycemic stability and provide antioxidants.
Practical, evidence-informed meal prep tips like batching grains, pre-chopping vegetables, and portioning single-serve dressings reduce decision fatigue and increase adherence.
Together, these strategies make it easier to sustain an anti-inflammatory pattern while fitting into busy weekly routines.
Anti-Inflammatory Breakfasts
How can morning choices help modulate systemic inflammation? Breakfast selections influence glucose, gut microbiota, and inflammatory markers; choosing nutrient-dense, low-glycemic options supports resolution pathways. Evidence favors whole grains, omega-3s, antioxidants, and fiber to reduce cytokine activity and improve metabolic signaling.
- Oat porridge with berries and ground flaxseed
- Greek yogurt with walnuts and turmeric-honey drizzle
- Smoothie: spinach, avocado, frozen berries, chia
- Whole-grain toast with mashed salmon and lemon
- Vegetable omelet with tomato, onion, and fresh herbs
These breakfasts align with clinical guidance to lower pro-inflammatory triggers while nourishing recovery.
Simple Meal Prep Tips
Planning meals for a week can reduce inflammatory drivers by stabilizing blood glucose, increasing fiber and omega‑3 intake, and limiting processed foods; evidence shows that consistent patterns of low‑glycemic, antioxidant‑rich meals lower cytokine activity and improve metabolic markers.
For simple meal prep, prioritize batch-cooking legumes, whole grains, roasted vegetables, and fatty fish or plant-based omega‑3 sources.
Use airtight containers, portion control, and a visible meal plan to avoid impulsive choices.
Prep sauces and dressings with turmeric, ginger, and olive oil.
Rotate colors and textures to maximize phytonutrients.
Label dates and freeze extras to maintain freshness and adherence.
10-Minute Meal-Prep Steps for the Week
Consistently, efficient minute-by-minute meal-prep steps reduce barriers to following an anti-inflammatory diet by decreasing decision fatigue and ensuring nutrient-dense choices are available throughout the week. The approach segments tasks into short, repeatable actions grounded in evidence-supported habits: batch-roast vegetables, portion lean proteins, pre-wash greens, cook whole grains, and prepare simple dressings. Small, timed routines increase adherence and preserve phytonutrients.
Tracking durations and temperatures minimizes nutrient loss and food safety risk. Visible, labeled containers support portion control and reduce impulsive choices. This method fosters sustainable behavior change through predictable, science-informed micro-tasks.
- Batch-roast mixed cruciferous vegetables
- Portion cooked legumes and proteins
- Pre-wash and spin leafy greens
- Cook grains in measured batches
- Whisk olive oil-based dressings
Budget Shopping for Anti-Inflammatory Ingredients
With modest adjustments to ordering and selection, shoppers can secure anti-inflammatory staples without exceeding a tight grocery budget. Prioritizing whole foods—beans, oats, canned tomatoes, frozen berries, and leafy greens—maximizes nutrient per dollar and supplies polyphenols, fiber, and omega-3 precursors.
Buying seasonal produce and bulk pulses reduces cost while supporting dietary diversity linked to lower inflammatory markers. Comparing unit prices, choosing store brands, and planning meals around sales minimizes waste and expenditure.
Simple meal templates that reuse cooked grains and legumes improve adherence and efficiency. Evidence-based budgeting preserves nutrient density and supports long-term dietary change without financial strain.
Flavor Hacks & Spice Blends to Boost Benefits
How can a few strategic spices and flavor techniques amplify the anti-inflammatory properties of everyday meals? Evidence links ingredients like turmeric, ginger, garlic and cinnamon to reduced inflammation markers; combining them with healthy fats and acid improves absorption and efficacy. Practical blends and methods make adherence easier and enhance nutrient bioavailability without extra calories.
- Toast spices briefly to release volatile oils and deepen anti-inflammatory potency.
- Pair turmeric with black pepper and coconut oil for curcumin uptake.
- Add grated ginger or garlic raw for allicin and gingerol benefits.
- Use citrus or vinegar to increase polyphenol stability.
- Rotate blends to target diverse pathways.
Troubleshooting Common Obstacles (Picky Eaters, Time, Cost)
What practical steps reduce barriers to adopting an anti-inflammatory meal plan? Practical, evidence-based strategies address picky eating, time, and cost while maintaining nutrient density. Offer gradual swaps, familiar flavors, and texture variations; batch-cook versatile bases; prioritize budget-friendly anti-inflammatory staples (beans, oats, frozen berries). Provide social support and simple recipes to increase adherence. Monitor preferences and adjust. The table below summarizes targeted tactics.
| Barrier | Practical tactic |
|---|---|
| Picky eaters | Introduce one new ingredient weekly |
| Time | Batch-cook 2–3 meals Sunday |
| Cost | Buy seasonal/frozen produce |
| Variety | Rotate spices and proteins |
Track Inflammation: Simple Markers and Symptom Signs
Regularly monitoring simple clinical markers and everyday symptoms helps gauge the inflammatory response to dietary changes and guides adjustments to an anti-inflammatory meal plan.
Objective measures such as CRP, fasting glucose, blood pressure and waist circumference complement subjective reports of pain, joint stiffness and energy.
Tracking trends over weeks informs whether increased omega-3s, fiber or antioxidant-rich foods produce measurable benefit.
Patients are encouraged to record baseline values, use repeat testing where appropriate, and report persistent or worsening signs to clinicians.
This approach aligns with evidence-based, patient-centered care that balances biochemical data with lived experience for targeted dietary refinement.
- C-reactive protein (CRP) levels
- Fasting glucose and HbA1c
- Blood pressure and waist circumference
- Pain, stiffness, and sleep quality logs
- Energy, mood, and gastrointestinal symptom tracking
Conclusion
Like a well-tended garden, an anti-inflammatory plate cultivates resilience: colorful vegetables, whole grains, fatty fish or legumes, and spices such as turmeric and ginger form the soil of better health. Practical pantry staples, simple breakfast templates, and budget strategies act as watering cans, while tracking symptoms provides sunlight for adjustments. Grounded in evidence and practical nurturing, this approach supports steady, measurable reductions in inflammatory risk and fosters sustainable dietary change over time.







